Prior to the introduction of Sentinel Lymph Node Biopsy (SLNB), the standard surgical staging of breast cancer involved complete Axillary Lymph Node Dissection (ALND). The procedure is effective in terms of local control but is associated with a high complication rate: upper extremity lymphedema in 20-30% of cases, impaired sensation, limited shoulder mobility, and chronic pain. SLNB has fundamentally changed this paradigm.
Concept and biological basis
The sentinel lymph node concept is based on the fact that lymphatic drainage from the tumor follows an anatomically predictable direction and reaches one or several “sentinels” - sentinel nodes - before spreading to other lymphatic structures. If the sentinel nodes do not contain metastases, the risk of the remaining axillary nodes being metastatic is low and axillary lymph node dissection can be avoided.
The method was introduced into clinical practice by Krag et al. and Giuliano et al. in the mid-1990s and has since been validated in numerous randomized trials. NSABP B-32 - one of the largest (5611 patients) - demonstrated that in the setting of a clinically negative axilla and negative sentinel node, SLNB achieved an equivalent oncologic outcome to ALND at a significantly lower morbidity.
Technique of execution
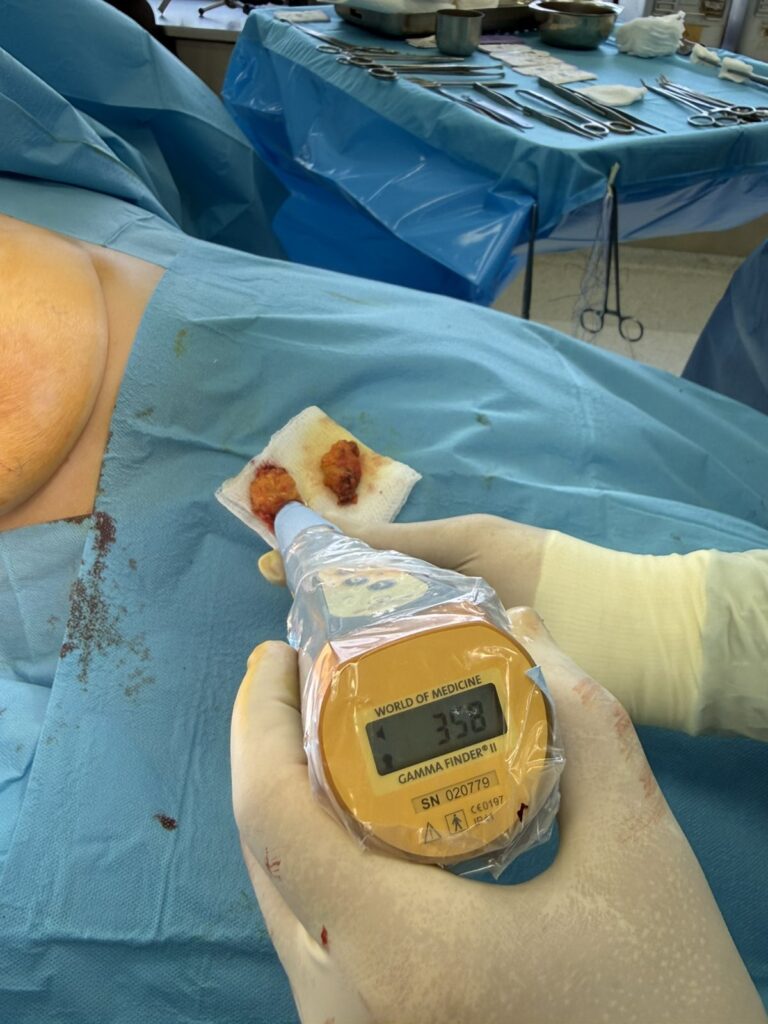
There are various methods of performing sentinel biopsies with the most widely used being radioisotope (Technetium-99m) and dye (Patent Blue or other blue dyes). Combining the two methods increases the identification rate to over 95% and reduces the false-negative rate to below 5-7%.
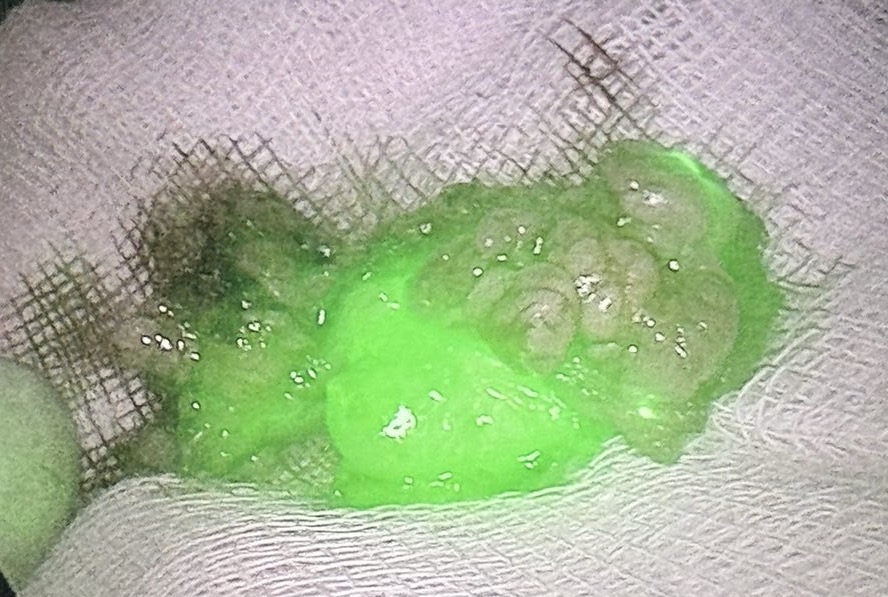
In recent years, the use of indocyanine green (ICG) with near-infrared fluorescence imaging has become widespread. The method is logistically more convenient as it does not require radioisotope retrieval, performance of SPECT-CT and patient stay in radiology department. It is performed at the time of surgery is connected and allows direct visualization of the lymph nodes.
When is SLNB the standard and when does ALND remain necessary?
In early breast cancer (T1-T2) with clinically negative axilla, SLNB is the undisputed standard by all current guidelines - NCCN (National Comprehensive Cancer Network), ESMO (European Society for Medical Oncology) and EUSOMA.
The landmark ACOSOG Z0011 study (Giuliano et al., 2011; 10-year data 2017) changed the approach even with limited axilla involvement. In patients with 1-2 positive sentinel nodes undergoing organ-sparing surgery and elective radiotherapy, axillary lymph node dissection did not improve local control, disease-free survival, or overall survival. Based on these data, ALND can be safely avoided in the majority of patients with micrometastases or single macrometastases in the sentinel node.
For mastectomy without planned radiotherapy or for 3 or more positive sentinel nodes, axillary lymph node dissection remains the standard approach.
Role of SLNB after neoadjuvant chemotherapy
The application of sentinel lymph node biopsy after neoadjuvant systemic therapy (post-NAC SLNB) is an active topic in clinical research. The SENTINA, SN FNAC, and ACOSOG Z1071 trials have shown that in patients who are initially clinically node positive (cN1) and achieve clinical axillary negation after NAC, SLNB is technically feasible with acceptable diagnostic accuracy-especially when using a dual tracer method and examining a minimum of 3 sentinel nodes. Clipping the positive node before NAC and its targeted excision (MARI - Marked Axillary Lymph Node Dissection, TAD - Targeted Axillary Dissection) further reduces the incidence of false-negative results.
Pathological evaluation - what does a “positive” sentinel node mean?
The classification of sentinel node involvement was standardized: isolated tumor cells (ITC, ≤0.2 mm), micrometastases (0.2-2 mm), and macrometastases (>2 mm). The clinical significance of ITCs and micrometastases is the subject of ongoing debate. The IBCSG 23-01 study showed that in patients with micrometastases in the sentinel node, ALND does not confer additional clinical benefit. In ITC, the consensus is that no ALND implementation is required.
Conclusion
Sentinel biopsy represents one of the most significant advances in the surgical treatment of breast cancer in the last three decades. It significantly reduces operative morbidity without compromising oncologic outcome. Current indications continue to expand thanks to data from prospective studies, and the introduction of new tracer technologies - such as ICG fluorescence - is making the method accessible to more and more surgical centers. Training in the proper performance of SLNB and correct interpretation of results are among the priorities of the Association of Breast Surgeons in Bulgaria.